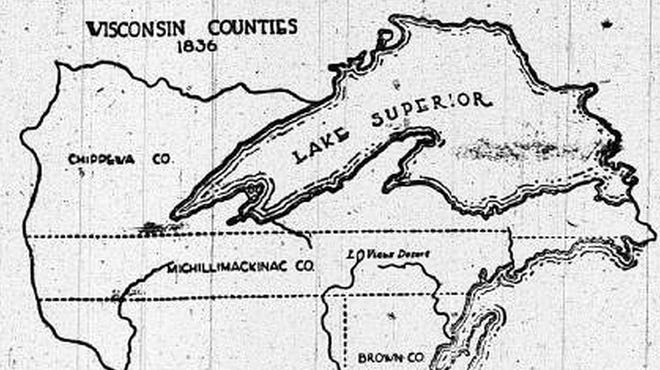
 Here's how Wisconsin got its name
Here's how Wisconsin got its name 3 Milwaukee playgrounds are hosting foam parties for kids this August
3 Milwaukee playgrounds are hosting foam parties for kids this August Noah's Ark will offer 3 Sensory Days in 2023
Noah's Ark will offer 3 Sensory Days in 2023 Here's what to know about Discovery World's two new exhibits
Here's what to know about Discovery World's two new exhibits Here's what to know about Six Flags Great America this summer
Here's what to know about Six Flags Great America this summer Here's where your kids can go to day camp in Milwaukee this summer
Here's where your kids can go to day camp in Milwaukee this summer  Meet the new 88-pound baby at the Milwaukee County Zoo
Meet the new 88-pound baby at the Milwaukee County Zoo A new harbor seal has arrived at the Milwaukee County Zoo
A new harbor seal has arrived at the Milwaukee County Zoo Giant robotic Ice Age animals will be at the zoo this summer
Giant robotic Ice Age animals will be at the zoo this summer This Mother's Day, I'm reflecting on what I signed up for
This Mother's Day, I'm reflecting on what I signed up for Here are things for families to do this spring in Milwaukee
Here are things for families to do this spring in Milwaukee 7 spring break camps, events and programs for kids in Milwaukee
7 spring break camps, events and programs for kids in Milwaukee Camp Timber-lee to remain open, Burn Camp will be held as planned
Camp Timber-lee to remain open, Burn Camp will be held as planned Camp Timber-lee in East Troy to close
Camp Timber-lee in East Troy to close Did Gordy the Groundhog see his shadow?
Did Gordy the Groundhog see his shadow? New exhibit with live animals teaches about evolution at museum
New exhibit with live animals teaches about evolution at museum Milwaukee County Zoo's new 15-foot anaconda is its longest snake ever
Milwaukee County Zoo's new 15-foot anaconda is its longest snake ever Milwaukee County Zoo introduces its longest snake, Olive
Milwaukee County Zoo introduces its longest snake, Olive What are the most nostalgic exhibits in the Milwaukee Public Museum?
What are the most nostalgic exhibits in the Milwaukee Public Museum? Here's what to know about Disney on Ice coming to Milwaukee
Here's what to know about Disney on Ice coming to Milwaukee Milwaukee County Zoo's Groundhog Day Celebration features Gordy again
Milwaukee County Zoo's Groundhog Day Celebration features Gordy again